
This blog was co-written by Anja Choon and Oyedeji Aderemi
Lassa fever, endemic in Nigeria and other African countries, is an acute viral haemorrhagic illness, which is mainly transmitted by rodents. Symptoms include fever, vomiting and diarrhoea. In severe cases, the disease also causes bleedings. It is estimated that 300,000 are infected each year in West Africa and that 5,000 of them die. Lassa fever kills more people than Ebola but receives much less attention.
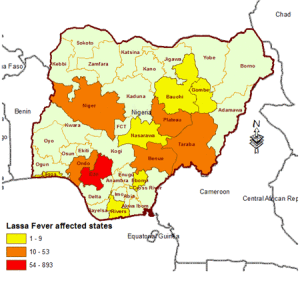
Even in Edo State, which has the highest prevalence of Lassa fever in Nigeria, most people seem to be unaware of this disease. Surveys administered in Uhiele-Ekpoma, Okada, Ogbese and Utese showed that only few had ever heard of Lassa fever. Among those that were aware, not everyone knew that rodents are the main source of infection. Most people falsely believed that mosquitoes transmit Lassa fever.
People in Edo State are exposed to many risk factors for Lassa fever. A survey in Esan West local government area showed that 96.1% of respondent had seen rodents inside their houses. As not everyone stored away food in rodent-proof containers, contamination with feces happened. In addition, many neither kept cooking utensils away from rodents nor washed them before use. Other risk factors such as eating possibly contaminated gari (a dish made from cassava tubers), frequenting traditional healers, touching corpses and hunting and eating rodents were also reported.
Apart from surveys, the researchers in Esan West also collected seroprevalence data, which would show the percentage of the population that had been infected by Lassa fever in the past. The seroprevalence observed in Esan West (58.2%) was much higher than that reported by other studies carried out in Nigeria (2% – 21.3%). Surprisingly, there was no significant link between seroprevalence and level of education, despite an earlier finding that knowledge of Lassa fever was better in people with a higher level of education.
All of these findings indicate that the current way of educating people in Nigeria, or at least Edo State, on Lassa fever is not efficient enough and needs to be adjusted. It’s clear that more effort has to be made so that everyone knows how Lassa fever can be transmitted and how to avoid transmission.
First Hand Narrative of a Fieldtrip to Study the Seroprevalence of Lassa Fever
During his usual work as a resident in family medicine at the Irrua Specialist Teaching Hospital, Dr. Oyedeji Aderemi sometimes sees patients with Lassa fever, who often present late, in the emergency room. The number of patients that come to this hospital with Lassa fever is substantial enough for a separate ward that almost never is completely empty. Part of the Irrua Specialist Teaching Hospital is also the Institute of Lassa Fever Research and Control. About three years ago, Dr. Oyedeji spent a week in the Lassa fever unit and participated in the above mentioned seroprevalence study in Esan West.

Dr. Oyedeji: “Doing research in Nigeria is fraught with a lot of challenges, especially when it comes to field work. I had first hand experience of this while collecting blood samples in a village in Edo State. The samples were going to be used to evaluate the seroprevalence of Lassa fever in that community.
The village where we worked is quite remote, and the roads that lead to it are in a terrible condition, like most roads connecting remote villages in Nigeria. This made it difficult for us to reach our field work site.
Language barrier was a big hurdle. The language of that community is Esan, which not everyone in our team spoke, which required us to work with interpreters. Still, we faced several challenges. One of them was that Esan does not have a word for Lassa fever. They call it and other illnesses ‘otagba’ and ‘ibafi’, which is seen as a spiritual attack. Recently, they have started to refer to Lassa fever as ‘the disease caused by rats’. The term is not so much in use yet, still it shows that people are becoming more aware that the illness is not caused by spirits but transmitted by rodents.
It was difficult to explain to the villagers that we wanted to investigate the Lassa seroprevalence in their community since ‘seroprevalence’, that is the presence of Lassa virus antibodies in their blood, does not have a direct translation either. We resolved to tell them that we wanted to find out if any of them presently had Lassa fever or carried it in their blood.
Some of the people we asked were reluctant to have their blood sample taken for screening, since the importance of the work was not readily understood by them, though several attempts were made to explain to them. They did not see how our research would be beneficial to them.
The village is an agrarian community, and community members are away from their homes working their farmland during the day. Hence, it was hard for us to locate them and consequently convince them to stop their work for a moment so that we could ask them questions and take blood samples.
While we were in the field, we also educated people on how Lassa fever is transmitted and how to protect themselves and their relatives. We explained the symptoms of Lassa fever to them and advised them to come to the hospital if they or someone else experiences these symptoms. Our hope is that this will increase early presentation of patients with Lassa fever at the hospital, which will help improve outcome.”

Comments